The 18 month sleep regression is a common period of disrupted sleep when a toddler who had been sleeping more predictably may suddenly resist bedtime, wake more at night, or become more upset around separation, often because of a combination of developmental and emotional changes happening at once. It’s widely recognized by parents, but like other regressions, it isn’t a precise milestone that every child hits on the same timeline.
If sleep has recently gotten harder, it can feel abrupt and confusing, especially if things had been going relatively smoothly. Around this age, though, a lot is shifting beneath the surface. Toddlers are more aware, more attached, and more independent all at once, and sleep is one of the places where those changes show up most clearly.
Key Takeaways
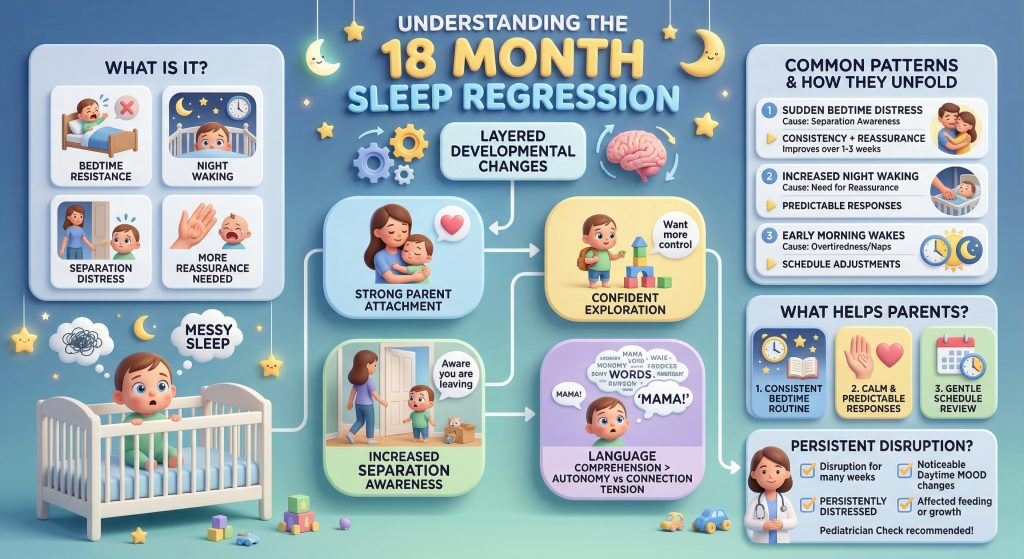
- The 18 month sleep regression is driven more by emotional development — separation awareness, independence, and attachment — than by sleep cycle changes.
- Common signs include bedtime resistance, increased night waking, early rising, and a stronger need for reassurance.
- Toddlers at this age need 11–14 hours of total sleep per day, typically split between one overnight stretch and one nap.
- Duration varies — some toddlers move through it in 1–2 weeks, others take longer, especially if routines shift during the disruption.
- Consistency and calm, predictable responses help more than overhauling everything at once.
Table of Contents
What is the 18 month sleep regression?
The term typically refers to a stretch of sleep disruption around 18 months that can include bedtime resistance, increased night waking, early rising, or a toddler who suddenly needs more reassurance to fall and stay asleep.
Unlike earlier regressions like the one around 8 months, this stage is less about sleep cycles themselves and more about how your child experiences separation, independence, and routine. As a result, sleep becomes less automatic and more relational, which is why it can feel different from earlier regressions.
Is the 18 month sleep regression real?
Many parents experience a clear shift in sleep around this age, so in that sense, it is very real. But it’s not a formal developmental marker that appears consistently for every child at exactly 18 months.
What’s more accurate is that this age brings together several changes that can affect sleep at the same time. For example, some toddlers move through this phase with only minor disruption. Others have a more noticeable stretch where bedtime becomes harder and nights feel less settled. The variation doesn’t mean one experience is more “correct” than another. It reflects how individual temperament, development, and routine interact.
What’s happening developmentally at 18 months?
Eighteen months is a particularly layered stage.
Toddlers at this age are:
- forming stronger attachments to caregivers
- becoming more aware of separation 5
- moving more confidently and exploring their environment
- understanding more language than they can express
Toddlers at this age need 11 to 14 hours of total sleep per day, typically split between one overnight stretch and one daytime nap 1,4.
That last piece is important. In particular, many toddlers can comprehend far more than they can say, which can lead to frustration, especially during transitions like bedtime. At the same time, their sense of independence is growing. In other words, they want more control, but they still rely heavily on connection. That tension, between wanting autonomy and needing closeness, often plays out most clearly at night.
What does the 18 month sleep regression look like?
It often feels like a shift from predictable sleep to something more emotional and less straightforward.
You might notice:
- stronger resistance at bedtime
- sudden distress when you leave the room
- more frequent night waking
- early morning wakeups
- a need for more reassurance than before
If sleep has been gradually shifting over weeks — shorter naps, later bedtimes, more resistance — it’s also worth gently revisiting the schedule.
What it looks like in practice
In real life, this can look like a toddler who was previously easy to put down suddenly crying when you leave, calling out repeatedly, or needing more time and presence to settle. However, the intensity can vary, so while for some children it’s a subtle change, for others there is a noticeable disruption that may impact the whole evening, and for many somewhere in between.
How long does the 18 month sleep regression last?
There isn’t a fixed duration, because this phase is not driven by one single cause. For some toddlers, it passes within a couple of weeks as they adjust to new developmental changes. For others, it can last longer, especially if sleep routines shift or if patterns around bedtime and night waking become more established.
Common patterns and how they tend to unfold
Separation awareness at its peak
Seeking connection overnight
Schedule or development shift
Daytime sleep out of balance
Separation awareness at its peak
Seeking connection overnight
Schedule or development shift
Daytime sleep out of balance
Swipe to compare
Some disruptions fade on their own, and others settle once the pattern around them becomes clearer.
Why sleep can feel especially hard at this age
This stage can feel more intense than earlier ones, even if the sleep disruption looks similar on paper. At 18 months, sleep can be just as much about emotionality as physicality. For instance, your toddler may now understand that you’re leaving and have stronger feelings around that. At this age, they likely don’t yet have the tools to fully process or manage that feeling. And that’s why bedtime can suddenly feel like a bigger transition. It’s not just about being tired, it’s about separation, control, and connection.
For parents, this can be one of the first times sleep feels like a negotiation rather than a routine. Consequently, that shift can be disorienting, especially if previous regressions felt more predictable.
What helps during the 18 month sleep regression?
What tends to help most at this stage is not a single technique, but a combination of steadiness and responsiveness. A consistent bedtime routine becomes especially important 2. If you’re still building those habits, our guide to establishing a sleep routine from the start covers the foundations that still apply at this age. It helps signal what’s coming next and gives your toddler something familiar to anchor to, even when emotions are running higher.
At the same time, many toddlers benefit from a bit more reassurance during this phase. That doesn’t mean changing everything about how sleep works, but it may mean acknowledging that your child needs more connection right now.
Additionally, it can also help to keep expectations simple. Not every protest needs to be negotiated, and not every moment of distress needs a new strategy. Often, what reduces friction over time is a calm, predictable response.
If sleep has been gradually shifting over weeks, shorter naps, later bedtimes, more resistance, it’s also worth gently revisiting the schedule. Small adjustments can sometimes make a noticeable difference. Research suggests the more consistently a bedtime routine is followed, and the earlier it’s established, the better children tend to sleep. 3
Every toddler’s sleep journey looks different at 18 months
Get a personalized plan based on your child’s age, sleep patterns, and what your family actually needs right now.
Take the 3-Min Sleep Quiz →What’s normal vs what may need more support
At this age, some level of resistance and increased emotion around sleep is typical.
It’s common to see:
- hesitation or protest at bedtime
- a stronger reaction to separation
- occasional night waking
- changes in nap behavior
Signs it may be time for extra support
It may be worth getting more support if:
- sleep disruption continues for many weeks without improvement
- your child seems persistently distressed or inconsolable
- there are noticeable changes in daytime mood, behavior, or development
- sleep is affecting feeding, growth, or overall well-being
This isn’t about labeling something as wrong. It’s about recognizing when additional guidance might be helpful.
What not to worry about
A harder stretch of sleep at 18 months doesn’t mean you’ve created a long-term problem and it doesn’t mean your toddler is regressing in a lasting way. You don’t have to overhaul everything immediately. This phase often reflects something important: your child is more aware, more connected, and more engaged with the world. As a result, sleep can get a little uneven as those changes settle. That’s part of development, not a sign that something is broken.
When to check with your pediatrician
It’s worth checking in if:
- your child seems physically uncomfortable at night
- there are signs of breathing issues, like snoring or pauses
- sleep disruption is extreme or worsening over time
- there are concerns about development, feeding, or growth
You don’t need a clear problem to ask a question. If something feels off, it’s reasonable to get input.
The American Academy of Sleep Medicine recommends that children aged 1 to 2 sleep 11 to 14 hours per 24 hours, including naps, and notes that regularly sleeping less is associated with attention, behavior, and learning difficulties.4
FAQs
Is the 18 month sleep regression caused by separation anxiety?
Separation awareness is one of the most common contributors at this age, but it’s rarely the only factor. Around 18 months, toddlers are becoming more aware that you can leave, and that awareness can make bedtime feel more emotionally charged. At the same time, they’re developing independence, language, and mobility, all of which can influence sleep.
What to watch for is how your child responds at separation. If bedtime distress centers around you leaving the room, separation may be a significant factor. What to do next is usually not to eliminate that reaction entirely, but to respond in a way that feels consistent and reassuring. Over time, predictability tends to help reduce intensity. If distress is severe or persists without improvement, it may be worth discussing with your pediatrician.
How long does the 18 month sleep regression last?
It varies. Some toddlers move through this phase in a week or two, while others take longer, especially if routines shift or sleep patterns become less consistent during the disruption. What to watch for is whether things are gradually settling or staying the same. A short-term spike in resistance often resolves as your child adjusts. If sleep has been difficult for several weeks without improvement, it may help to look more closely at bedtime routines, nap timing, and how sleep is supported. What to do next depends on that pattern. If things are easing, staying steady may be enough. If not, small, consistent adjustments tend to be more effective than large changes.
Why is my 18 month old suddenly waking up at night?
Night waking at this age is often tied to increased awareness and a stronger need for reassurance. Your toddler may now fully register that you’re not there and call out or wake more easily as a result. It can also be influenced by changes in routine, nap timing, or overall sleep balance during the day. What to watch for is whether the waking seems emotional, habitual, or related to discomfort. Emotional waking often comes with calling out or distress. Habit-based waking may follow a consistent pattern. Physical discomfort usually has other signs alongside it.
What to do next depends on the cause. Consistency in how you respond overnight often helps reduce repeated waking over time. If waking is frequent, intense, or paired with other concerns, it’s reasonable to check in with your pediatrician.
Is this the same as the 2 year sleep regression?
They’re related, but not identical. The 18 month phase tends to be more about attachment and separation awareness, while The 2 year stage often includes more boundary testing, independence, and negotiation – you can read more in our guide to 2 year milestones and what to expect at 24 months.
At 18 months, sleep disruption often feels more emotional. At 2 years, it often feels more behavioral. Some children experience both. Others move through one more noticeably than the other.
If your toddler is closer to two and sleep has shifted again, our dedicated 2 year sleep regression guide covers what to watch for and how to respond.
Did I cause the 18 month sleep regression?
No. This phase reflects normal developmental changes, not a single parenting decision. Sleep at this age is influenced by developmental growth, emotional awareness, routine changes and temperament, among other factors.
It’s common to wonder if responding differently would have prevented the disruption. In most cases, that’s not how it works.
What matters more is what you do next. Toddlers are adaptable, and sleep patterns can shift with steady, consistent support. If you feel stuck or unsure, guidance from your pediatrician can help you move forward with more clarity.
Should I change how I respond at bedtime?
You don’t necessarily need to change everything, but it can be helpful to reflect on whether your current approach feels sustainable and consistent. If your toddler seems to need more reassurance right now, offering that within a predictable structure can help. If bedtime has become drawn out or inconsistent, gently tightening the routine can reduce confusion. What to watch for is whether your approach is helping things settle over time. What to do next is usually about small adjustments rather than a complete reset.
Sleep at 18 months is emotional, not just physical
Betteroo builds a plan around your toddler’s age, temperament, and what your family is actually going through — so you can respond with confidence instead of guesswork.
Take the Free Sleep Quiz →5 Sources
- Hirshkowitz, M., et al. (2015). National Sleep Foundation’s updated sleep duration recommendations: final report. Sleep Health, 1(4), 233–243. https://pubmed.ncbi.nlm.nih.gov/29073398/
- Mindell, J.A., & Williamson, A.A. (2018). Benefits of a bedtime routine in young children: Sleep, development, and beyond. Sleep Medicine Reviews, 40, 93–108. https://pubmed.ncbi.nlm.nih.gov/29195725/
- Mindell, J.A., et al. (2015). Bedtime routines for young children: a dose-dependent association with sleep outcomes. Sleep, 38(5), 717–722. https://pubmed.ncbi.nlm.nih.gov/25325483/
- Paruthi, S., et al. (2016). Consensus Statement of the American Academy of Sleep Medicine on the Recommended Amount of Sleep for Healthy Children. Journal of Clinical Sleep Medicine, 12(11), 1549–1561. https://pubmed.ncbi.nlm.nih.gov/27707447/
- American Academy of Pediatrics — HealthyChildren.org. How to Ease Your Child’s Separation Anxiety. https://www.healthychildren.org/English/ages-stages/toddler/Pages/Soothing-Your-Childs-Separation-Anxiety.aspx









