If you’ve Googled “does sleep training work” you’ve gotten one of two answers: the pro side calls it scientifically proven, the anti side calls it harmful. Both are misreadings of the actual research.
Key Takeaways
- There is strong evidence sleep training improves sleep. In randomized trials of babies 4 months and older, formal sleep training improves both infant sleep and parent mental health without measurable long-term harm.
- Compelling safety data: Price 2012 followed sleep-trained children for 5 years and found no differences from controls on attachment, behavior, or cortisol patterns.
- The 2012 Middlemiss cortisol paper is often cited as evidence against sleep training, however uncertainty arises as it had only 25 babies, no control group, and 2 days of cortisol data.
- The evidence is most compelling for graduated approaches like the Ferber method, controlled crying, and bedtime fading.
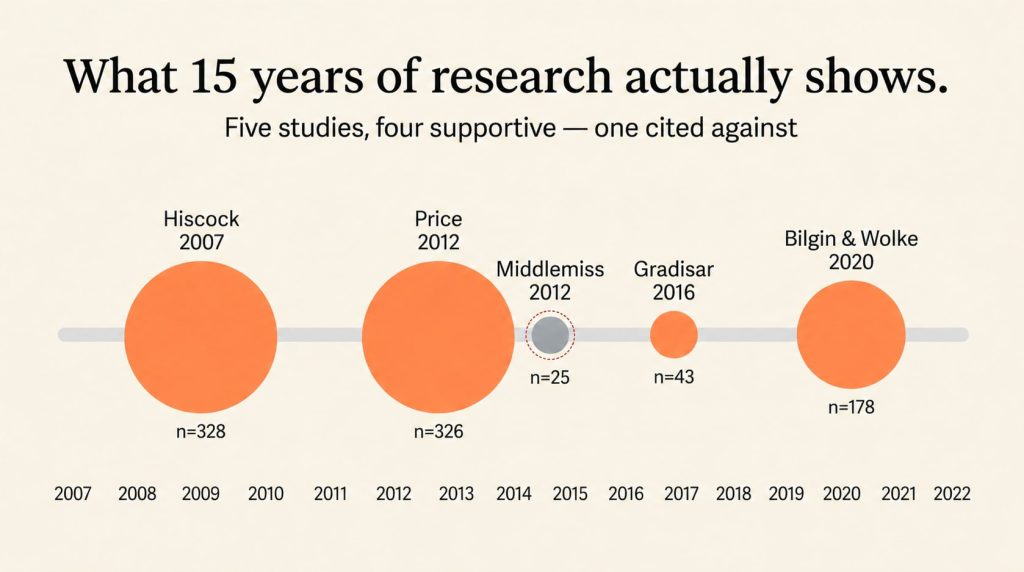
Roughly 30 randomized or controlled trials exist on behavioral sleep interventions in infancy, plus a handful of long-term follow-ups. Five do most of the heavy lifting in public conversation – four supportive, one repeatedly cited against. This is designed to provide reassurance of the evidence we have on that question.
Table of Contents
What 4 major sleep training studies actually found
Hiscock et al., 2007 (BMJ) – cluster RCT, n=328
What it found: Sleep training in 7-month-olds reduced both baby wake-ups and maternal depression at 12-month follow-up. The biggest effect was on mothers, not babies.
A cluster-randomized trial across 49 health centers in Melbourne. 328 mothers of 7-month-olds with reported sleep problems were randomized to a controlled-crying or camping-out intervention, or to usual care. At 12 months, the intervention group had fewer sleep problems and significantly lower maternal depression rates.¹ Controlled crying is the same family of graduated approach the Ferber method is built on – one of several common sleep training methods parents consider. Most pro-sleep-training writing buries the maternal-mental-health finding, but it’s the headline.
Price et al., 2012 (Pediatrics) – 5-year follow-up of the Hiscock cohort
What it found: Five years later, sleep-trained children were indistinguishable from controls on attachment, behavior, cortisol, and emotional wellbeing. This is one of the most reassuring pieces of evidence we have on the question of is it causing harm.
Followed the same cohort up at age six (326 children selected, 173 from the intervention arm). Researchers measured emotional and behavioral functioning, parent-child closeness, disinhibited attachment, cortisol, and child-reported wellbeing. They found no significant differences between groups on any measure² – including no difference on disinhibited attachment, the outcome that addresses the most common worry. The longest and most rigorous follow-up the field has.
Gradisar et al., 2016 (Pediatrics) – RCT, n=43
What it found: Both graduated extinction and bedtime fading improved sleep, lowered cortisol (didn’t raise it), and left attachment unchanged. This is a powerful takeaway in that it is not consistent with the concerns many parents have heard.
Randomized 43 infants (6-16 months) to graduated extinction, bedtime fading, or a sleep-education-only control. Both intervention groups showed significant improvements in sleep latency and night wakings compared with control. Salivary cortisol showed small-to-moderate declines in both intervention groups compared with control.³ At 12-month follow-up, no differences emerged between groups on emotional and behavioral problems or on secure-versus-insecure attachment styles. Smaller sample than Hiscock, but a tighter design – and the cleanest cortisol data we have.
Bilgin & Wolke, 2020 (J Child Psychology and Psychiatry) – longitudinal cohort, n=178
What it found: Families using “cry it out” approaches showed no differences in attachment or behavior at 18 months versus families who didn’t – even when the sample included preterm babies.
A longitudinal observational study following 178 mother-infant dyads (105 full-term and 73 very preterm / very low birthweight) across the first 18 months. Researchers compared families who used “cry it out” approaches with families who didn’t, measuring attachment security and behavioral development at 18 months. They found no adverse effects on either outcome.⁴ Not a randomized trial – but at this sample size, with that endpoint, it adds an independent line of evidence to Price 2012’s 5-year findings on attachment.
Why we trust these four (and one important caveat)
These studies are generally considered more reliable because they use larger samples and, in several cases, randomized designs. Bilgin & Wolke is observational but at a scale that adds useful corroboration to the randomized attachment findings.
One caveat. These studies tested specific protocols – graduated extinction, controlled crying, bedtime fading, camping out. They don’t validate every method called “sleep training” today, particularly more aggressive full-extinction commercial programs. The evidence base is for graduated approaches, not for every sleep training app or program sold under the same label.
Wondering if sleep training is right for your baby?
Take Betteroo’s 3-minute quiz to see what fits your baby, your capacity, and your family.
Take the 3-Min Quiz →The one study cited against – and why it can’t carry that weight
Middlemiss et al., 2012 (Early Human Development) – inpatient study, n=25
What the study claimed: On the third day of an extinction-based inpatient program, infants stopped crying behaviorally but their cortisol stayed elevated. Anti-sleep-training pieces interpret this as “hidden distress.”⁵
Why it’s important to interpret this study carefully: It’s often asked to answer questions that are larger than what the study itself was designed to address. The study included 25 infants, had no control group, and measured cortisol over a very short window. Because of these limitations, it’s difficult to draw broader conclusions from it on its own.
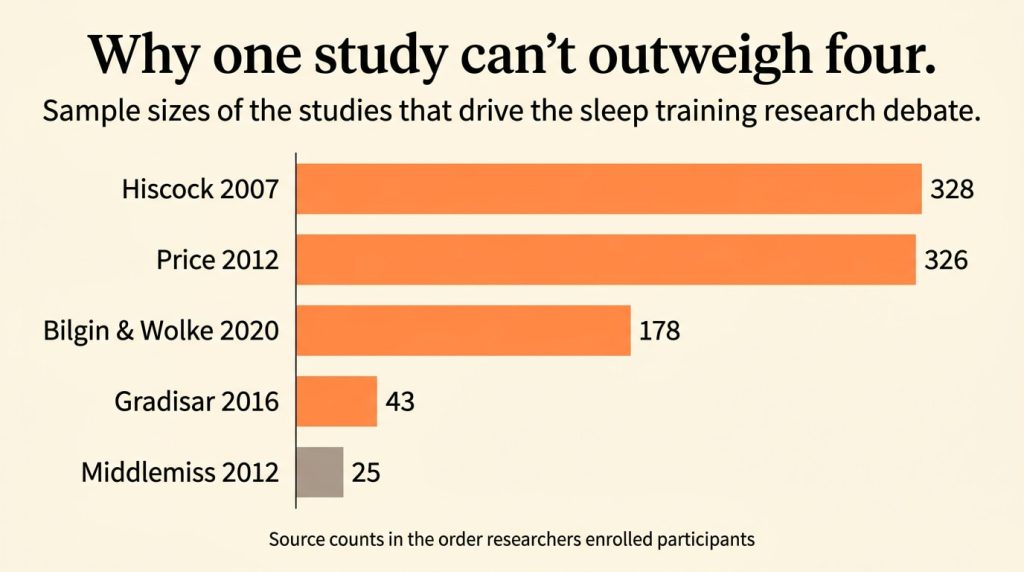
This isn’t a takedown of the researchers. It’s a reminder that one paper of n=25 with no control group cannot tell you whether sleep training is harmful. When a single small study is doing all the persuasive work in a public conversation, that is itself a signal to be skeptical – of the conclusion, not just the study.
What the research can’t tell us
Almost all sleep-training research is on babies older than four months – there’s little evidence base for younger infants, and most pediatric experts agree formal sleep training isn’t appropriate before that age regardless. Most studies measure outcomes in weeks or months, not years; the longest follow-up the field has is Price 2012 at five years. Few studies compare methods head-to-head, so we can’t say Ferber works better than bedtime fading or the chair method – most claims about method superiority track consistency of execution, not the protocol.
Baby temperament as a moderator is barely studied – clinicians know some babies respond easily and others don’t, but the literature mostly ignores it. The cortisol question is genuinely unsettled – other studies (Gradisar 2016³; Hall et al. 2015⁶) have found no cortisol elevation after sleep training. The picture is messy and underpowered, not closed.
Frequently asked questions
Is sleep training safe?
For babies 4 months and older, the largest randomized trials and a 5-year follow-up found no measurable harm. The evidence base is for graduated approaches – controlled crying, bedtime fading, the chair method – not aggressive full-extinction commercial programs. Under 4 months, formal sleep training isn’t appropriate regardless of method.
Does sleep training cause attachment problems?
The best available evidence does not show this. Price 2012 specifically measured attachment outcomes 5 years after sleep training and found no differences from controls. Bilgin & Wolke 2020 reached the same conclusion at 18 months in an independent cohort. Two separate lines of evidence, same answer.
What about the cortisol study people keep mentioning?
That’s the 2012 Middlemiss study – 25 babies, no control group, two days of cortisol data, no replication. Other studies (Gradisar 2016, Hall 2015) found no cortisol elevation after sleep training. The cortisol question is genuinely unsettled – not closed in either direction.
What age does the research support sleep training?
4 months and older. There’s almost no evidence base for younger infants, and most pediatric experts don’t recommend formal sleep training before 4 months regardless of method – which is also when many families first hit the 4-month sleep regression. Under 4 months, the work is building conditions – consistent wind-down, day sleep, feeding adequacy – not running a protocol.
What if sleep training doesn’t work for my baby?
It’s a real and underserved subset. Some babies don’t respond to graduated approaches even when parents stay consistent for 14 nights. Three things to consider: switch to a gentler method (some babies do better with bedtime fading than Ferber), check for medical contributors that mimic sleep problems (silent reflux, allergies, sleep-disordered breathing), or wait – some babies physiologically aren’t ready until later. “It didn’t work” is data, not failure.
Key takeaway
If you read one sentence from the research: in randomized trials with babies four months and older, formal sleep training improves sleep and parent mental health without measurable long-term harm. There are real gaps, and babies who don’t respond to any protocol. But the case that sleep training is intrinsically harmful is based largely on a small number of limited studies, rather than the broader body of research. It’s not a perfect answer, but it’s the most balanced one we have right now.
Still not sure where you stand?
Take Betteroo’s 3-minute quiz for a personalized read on whether sleep training is right for your family – and which approach fits.
Get Personalized Sleep Help →6 Sources
- Hiscock, H., Bayer, J., Gold, L., Hampton, A., Ukoumunne, O.C., & Wake, M. (2007). Improving infant sleep and maternal mental health: a cluster randomised trial. BMJ, 335(7611). https://pubmed.ncbi.nlm.nih.gov/17158146/
- Price, A.M.H., Wake, M., Ukoumunne, O.C., & Hiscock, H. (2012). Five-Year Follow-up of Harms and Benefits of Behavioral Infant Sleep Intervention: Randomized Trial. Pediatrics, 130(4), 643–651. https://pubmed.ncbi.nlm.nih.gov/22966034/
- Gradisar, M., Jackson, K., Spurrier, N.J., et al. (2016). Behavioral Interventions for Infant Sleep Problems: A Randomized Controlled Trial. Pediatrics, 137(6), e20151486. https://pubmed.ncbi.nlm.nih.gov/27221288/
- Bilgin, A., & Wolke, D. (2020). Parental use of ‘cry it out’ in infants: no adverse effects on attachment and behavioural development at 18 months. Journal of Child Psychology and Psychiatry, 61(11), 1184–1193. https://pubmed.ncbi.nlm.nih.gov/32155677/
- Middlemiss, W., Granger, D.A., Goldberg, W.A., & Nathans, L. (2012). Asynchrony of mother-infant hypothalamic-pituitary-adrenal axis activity following extinction of infant crying responses induced during the transition to sleep. Early Human Development, 88(4), 227–232. https://pubmed.ncbi.nlm.nih.gov/21945361/
- Hall, W.A., Hutton, E., Brant, R.F., et al. (2015). A randomized controlled trial of an intervention for infants’ behavioral sleep problems. BMC Pediatrics, 15:181. https://pubmed.ncbi.nlm.nih.gov/26567090/









